|
Maximal viral suppression often takes longer in patients with higher baseline HIV RNA levels (e.g., greater than 100,000 copies per mL). 6, 7 Failure to achieve the target level of less than 50 copies per mL after 16 to 24 weeks of treatment should prompt consideration of drug resistance, inadequate drug absorption or poor compliance. A typical goal is a 1- to 2-log reduction within four to eight weeks (e.g., from 50,000 copies per mL to 500 copies per mL). Guidelines on the expected PVL reductions vary. 22 Ideally, the HIV RNA level should decline rapidly after antiretroviral drug therapy is initiated. 
As mentioned previously, a minimum of two CD4+ cell counts and PVL measurements should be obtained on separate visits before treatment is changed. PVL testing may be helpful in the rare instance of indeterminate HIV antibody testing, especially in a patient with recent infection.ĬD4+ cell counts and HIV RNA levels are important tools for evaluating treatment response. 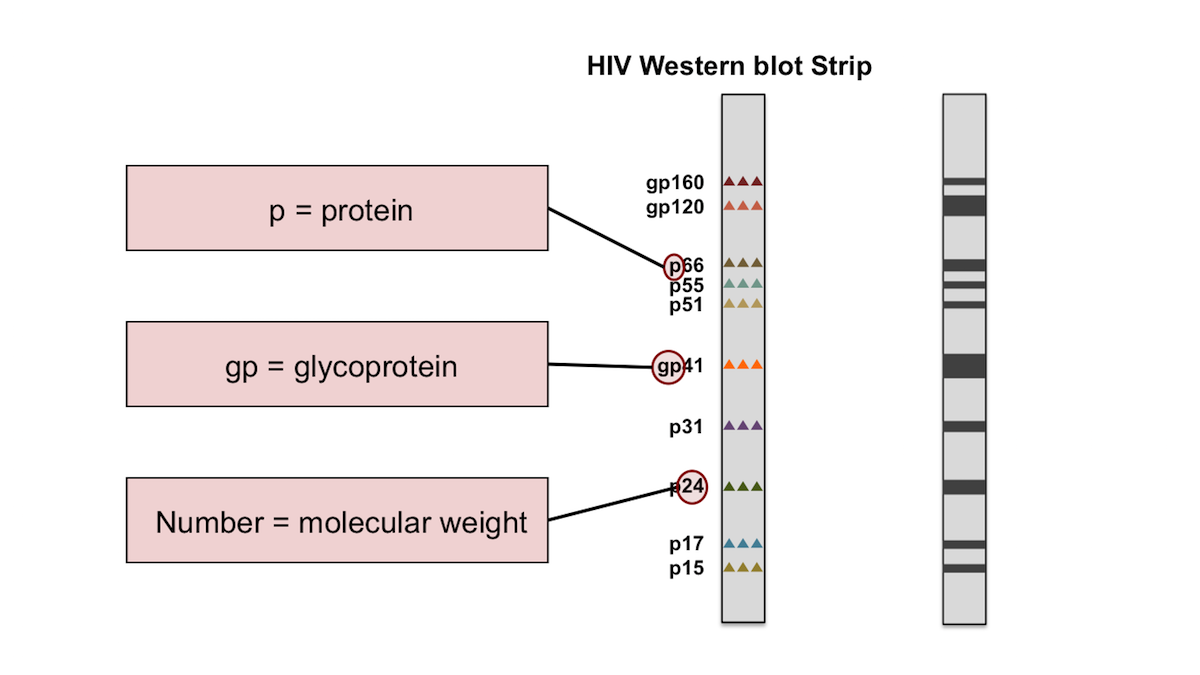
At least two PVL measurements usually should be performed before antiretroviral drug therapy is initiated or changed. When feasible, the same assay should be used for serial PVL testing in the individual patient. Periodic monitoring of PVL is important to promptly identify treatment failure. The goal is no detectable virus in 16 to 24 weeks. PVL levels usually show a 1- to 2-log reduction within four to six weeks after therapy is started. Initiation of antiretroviral drug therapy is usually recommended when the PVL is 10,000 to 30,000 copies per mL or when CD4+ T-lymphocyte counts are less than 350 to 500 per mm 3 (0.35 to 0.50 × 10 9 per L). Plasma viral load (PVL) testing has become a cornerstone of HIV disease management. Interpretation of the WB band pattern in combination with clinical features may be occasionally useful in predicting the stage of HIV infection.The polymerase chain reaction assay, branched DNA assay and nucleic acid sequence-based amplification assay quantitate human immunodeficiency virus (HIV) RNA levels. Correlation of CD4 cell counts with the various uncommon band patterns showed that only 5.56% (4/72) had counts in the 200-500 cells/microl range, whereas 45.83% and 48.61% had counts of 500 cells/microl respectively. On classifying the WB reactive cases by the WHO clinical staging system, 38.45% (564/1467) were in Stage 1, 47.99% (704/1467) in stages 2 and 3 and 13.56% in stage 4. Of all individual bands, p31 band was the most frequently missing one, absent in 7.09% cases. Reactivity with all the bands was the most commonly observed WB pattern, occurring in 92.91% (1363/1467) of cases, whereas the other 7.09% showed uncommon band patterns.  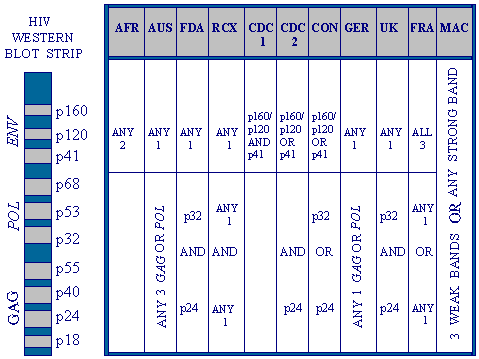
For the interpretation of the WB results in this study, the guidelines recommended by NACO, India were followed. We performed a retrospective study with 1,467 HIV-1 infected cases confirmed by WB test between January 2002 to July 2005, with the objective of mapping different band patterns of western blot results and determining whether the presence or absence of certain bands was associated with any specific stage of HIV infection. Mapping different band patterns of Western blot results and correlating them with stages of HIV infection. Although the overall sensitivity and specificity of the western blot (WB) test for detection of antibodies to various viral proteins is high, there has been a substantial difference in the timing of the appearance of antibody bands and their intensities during different stages of HIV infection.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
